Electron microscopy image of the SARS-CoV-2 virus.
COVID-19 Infection Statistics
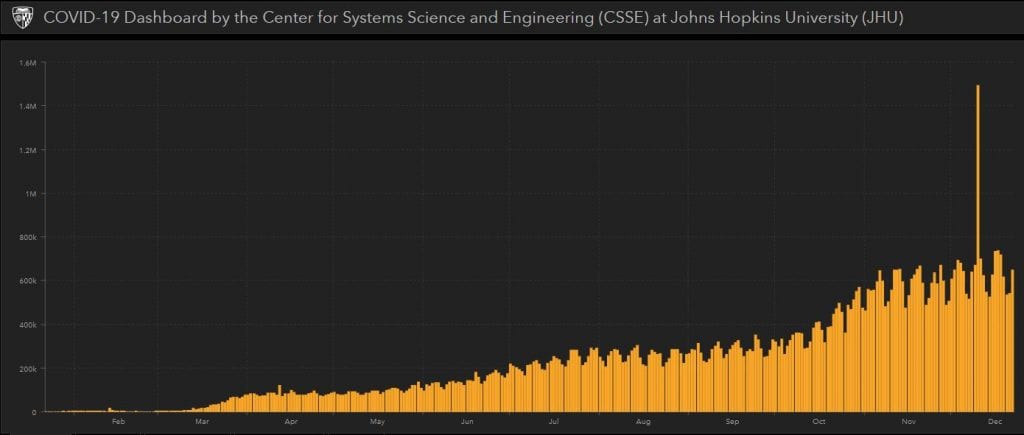
Although anti-COVD vaccines are rolling out and people are being immunized, as of early late December 2020, the rate at which daily, newly reported COVID-19 cases has continued to rise (Figure 1). In my 29 June 2020 What’s New article I discuss some of the limitations of such global statistics. In that post, I argued that the statistics would be more meaningful if the U.S. Centers for Disease Control’s (CDC’s) morbidity and mortality reporting standards were used. Apropos of COVID-19, morbidity refers to patients’ cases reported and having the disease and mortality refers to COVID-19 patients who die from their COVID-19 infection. Both morbidity and mortality are reported as ratios of incidence per 100,000 potentially exposed individuals. I illustrated this in my portion of an STLE webinar presented in July 2020.
What Do the Infection Statistics Mean?
Social scientists, epidemiologists, and public health specialists continue to debate the details, but the general consensus is that the disease spreads most widely and rapidly when individuals ignore the fundamental risk-reduction guidelines. It appears that COVID 19 communicability is proportional to the number of SARS-CoV-2 virus particles to with individuals are exposed. Figure 2 illustrates the relative number of virus particles shed during the course of the disease.
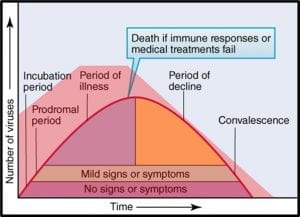
Notice that the number of viruses shed (or dispersed by sneezing, coughing, talking, and breathing) is quite large early on – before symptoms develop fully. It’s a bit more complicated than that, however. Not all infected individuals are equally likely to shed and spread the virus. All things being apparently equal, some – referred to as super-spreaders – are substantially more likely than others to infect others. Although people with or without symptoms can be super-spreaders, those who are infected but asymptomatic are particularly dangerous. These folks do not realize that they should be self-quarantining. A study published in the 06 November 2020 issue of Science (https://science.sciencemag.org/content/370/6517/691) reported that epidemiological examination of millions of COVID-19 cases in India revealed that 5 % of infected people were responsible for 80 % of the reported cases.
What Shall We Do While Waiting for Herd Immunity to Kick-In?
The best strategy for avoiding the disease is to keep yourself physically distanced form others. Unfortunately, this advise is all but worthless for most people. We use public transportation to commute to work. We teach in classrooms, work in offices, restaurants, medical facilities, and industrial facilities in which ventilation systems are unable to exchange air frequently enough to minimize virus exposure risk. The April 2020 ASHRE Position Document on Infectious Aerosols recommends the use of 100 % outdoor air instead of indoor air recirculation. The same document recommends the used of high-MERV (MERV – minimum efficiency removal value – 10-point scale indicating the percentage of 0.3 µm to 10 µm particles removed) or HEPA (HEPA – high efficiency particulate absorbing – able to remove >99.9% of 0.3µm particles from the air) filters on building HVAC systems. Again, as individuals who must go to work, shop for groceries, etc., outside our own homes, we have little control over building ventilation systems.
Repeatedly, CDC (Centers for Disease Control), HSE (UK’s Health and Safety Executive), and other similar agencies have offered basic guidance:
1. Wear face masks – the primary reasons for doing this is to keep you from transmitting aerosols and to remind you to keep your hands away from your face. Recent evidence suggests that that although masks (except for ones that meet N-95 criteria) are not very efficient at filtering viruses out of the air inhaled through them, they do provide some protection.
2. Practice social distancing to the extent possible. The generally accepted rule of thumb is maintaining at least 6 ft (1.8 m) distance between people. This is useful if you are in a well-ventilated space for relatively short periods of time but might be insufficient if you are spending hours in inadequately ventilated public, industrial, or institutional spaces.
3. Wash hands thoroughly (at least 30 sec in warm, soapy water) and frequently. The objective here is to reduce the chances of first touching a virus laden surface and then transferring viruses into your eyes, nose, or mouth.
Here are links to the most current guidance documents:
CDC – How to Protect Yourself and Others – https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/prevention.html
CDC – Interim Guidance for Businesses and Employers Responding to Coronavirus Disease 2019 (COVID-19), May 2020 – https://www.cdc.gov/coronavirus/2019-ncov/community/guidance-business-response.html
HSE – Making your workplace COVID-secure during the coronavirus pandemic – https://www.hse.gov.uk/coronavirus/working-safely/index.htm
UKLA- HSE Good Practice Guide – http://www.ukla.org.uk/wp-content/uploads/HSE-Good-Practice-Guide-Sept20-Web-LowresC.pdf – discusses health & safety in the metalworking environment.
WHO – Coronavirus disease (COVID-19) advice for the public – https://www.who.int/emergencies/diseases/novel-coronavirus-2019/advice-for-public
Remember: Prevention really Means Risk Reduction
It is impossible to reduce the risk of contracting COVD-19 to zero. However, timely and prudent preventative measures can reduce the risk substantially so that people can work, shop, and interact with one another safely. Guidance details continue to evolve as researchers learn more about SAR-CoV-2 and its spread. However, the personal hygiene basics have not changed since the pandemic started a year ago. If each of us does our part, we will be able to reduce the daily rate of new cases dramatically, long before the majority of folks have been immunized.
For more information, contact me at fredp@biodeterioration-control.com

